Arise Chiropractic and Wellness Chiropractic Blog
What Is Chiropractic in Vernon?
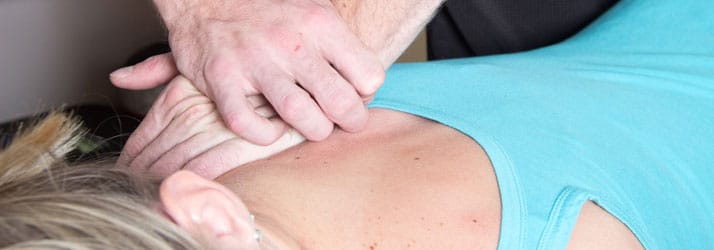
What Is Chiropractic in Vernon? There are many different styles and techniques in the chiropractic field, but they all have a common goal. That goal is to assess, detect and correct spinal misalignment and to improve posture, nerve, muscle, and organ function. Chiropractors in Vernon make adjustments to the alignment through a series of impulses…
What’s the Tea? (4 T’s to Be Mindful Of) in Vernon
What’s the Tea? (4 T’s to Be Mindful Of) in Vernon Apparently, the term “What’s the tea?” or “Spill the tea” is an old expression from the 18th century that women used to say when sharing gossip. This old expression has gained a lot of traction with millennials and Gen Z as new (or, rather,…
Why Choose Chiropractic Care in Vernon
Why Choose Chiropractic Care in Vernon Chiropractic treatment is a viable solution for many different health issues. Whether you have a bulging disc in your back, debilitating back pain, or you suffer from severe headaches several times per week, seeing a chiropractor can help. The key is to find the right chiropractor for your personality…
Vernon Chiropractic Clinic Talks About Bulging Discs
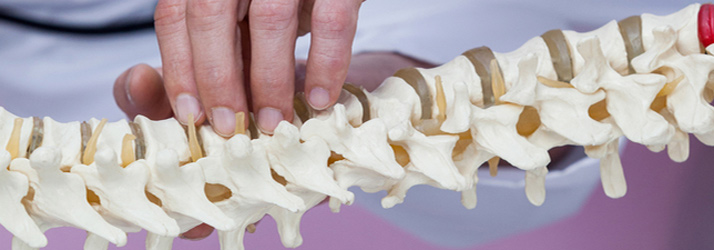
Vernon Chiropractic Clinic Talks About Bulging Discs Have you ever heard of a slipped disc? It’s a misnomer. Discs never “slip”, but they can bulge. When they do a Vernon chiropractor may be able to help. Intervertebral disc disorders are referred to as “contained” or “non-contained.” A bulging disc is considered a contained disc disorder.…
Vernon Chiropractic Helps Auto Accident Patients
Vernon Chiropractic Helps Auto Accident Patients If you are ever unlucky enough to be injured in a car accident you may experience a strain of your neck muscles and the surrounding soft tissue. The feeling is called whiplash and it can limit your neck movement severely. When a vehicle is hit from the rear (or the…
Vernon Chiropractic Clinic Explains the Value of Health
Vernon Chiropractic Clinic Explains theValue of Health The human body is designed to naturally repair itself, but it is an ability that is dependent on a healthy nervous system. Our Vernon chiropractor offers safe and painless corrections that can help your body heal faster and prevent disease. Your spine is the key pillar of your…